The Second Wave
Nepal is in the beginning of the second wave of the COVID-19 pandemic. If you want to know how bad the second wave potentially can get in Nepal, you just need to look across the border to India.
What happens in India, happens in Nepal. An open border with free movement of people means the two countries are essentially part of the same epidemiologic unit for infectious disease transmission. In addition to an open border, the two countries also share common biological, sociocultural, behavioral, and environmental characteristics that contribute to infectious disease transmission.
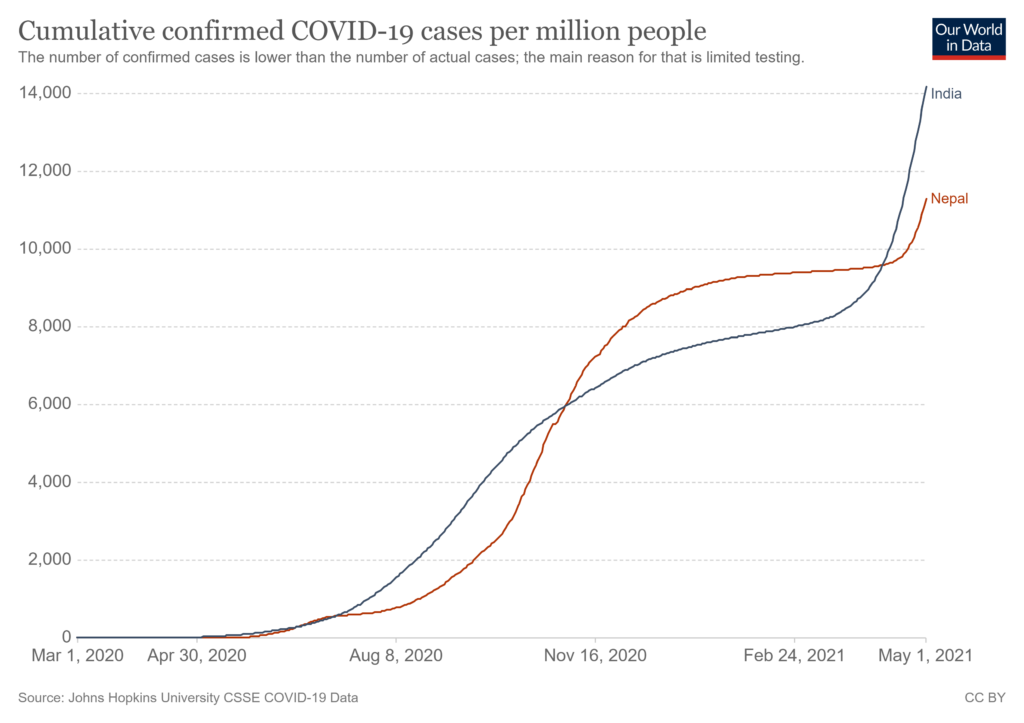
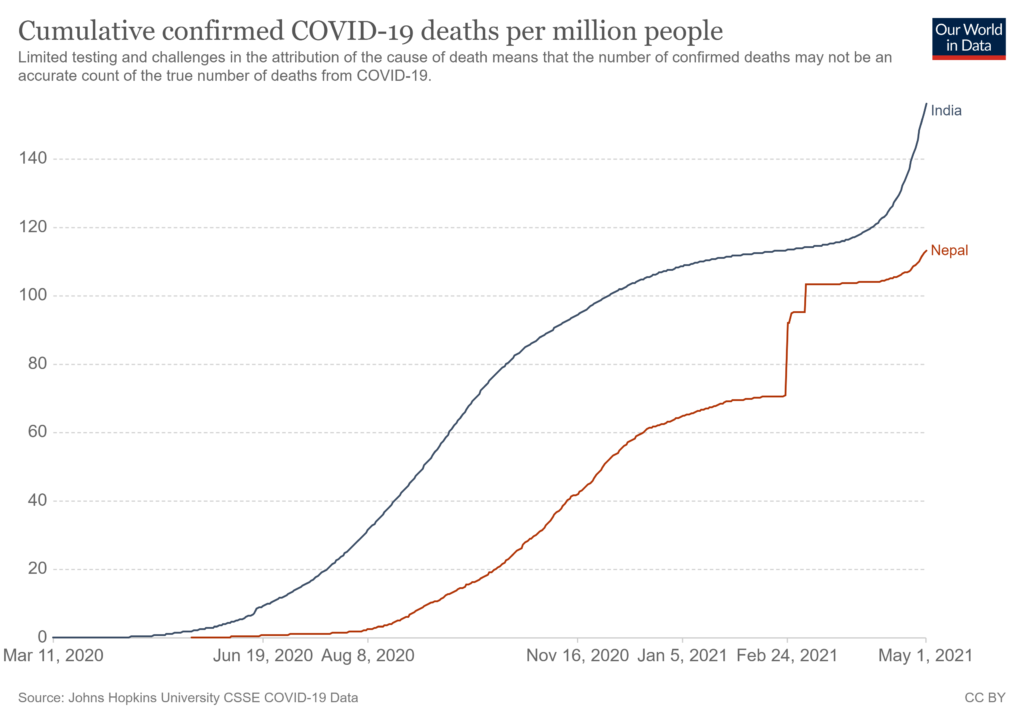
India is in the throes of a devastating second wave of the COVID-19 epidemic with daily reported cases averaging over 370,000 and daily deaths averaging over 3,300 this the past week. The total reported cases in India have surpassed 19 million and deaths 215,000. The situation in India is going to get worse before it gets better and portends things to come in Nepal providing warning for Nepal to act swiftly to prevent a similar scenario.
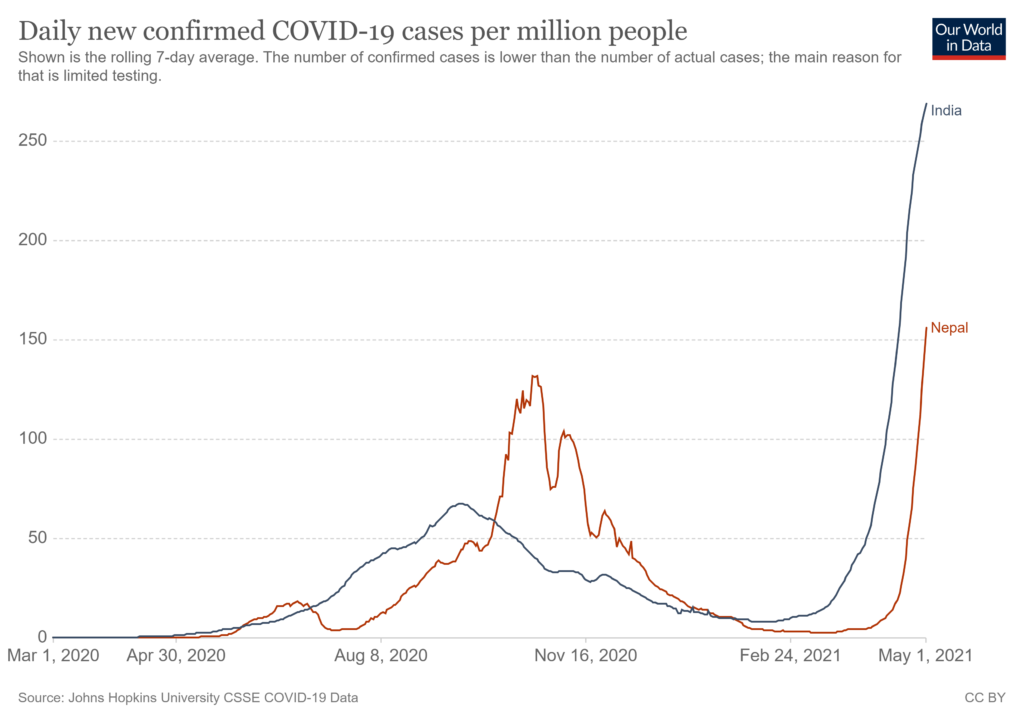
On May 1, 2021, Nepal had the highest 7-day average of the daily reported COVID-19 cases (4,543) since the pandemic started over a year ago. As of May 1, 2021, the total number of reported COVID-19 cases and deaths in Nepal were almost 329,000 and 3,300, respectively. The reported COVID-19 cases and deaths in both countries are likely a gross underestimate of true statistics due to a lack of adequate COVID-19 testing, and medical certification and registration of a large proportion of deaths.
The population of India is almost 47-times larger than the population of Nepal. Therefore, the absolute number of COVID-19 cases and related deaths in India are going to be substantially higher than Nepal. However, on a per capita basis, the epidemic trends in the two countries are very similar in terms of infections and deaths.
Nepal’s COVID-19 epidemic is following India’s trajectory and is now behind by only a couple of weeks. Nepal’s 7-day average of 156 cases per 1 million people on May 1, 2021 was where India stood on April 17, 2021. A week ago, Nepal’s epidemic was about three weeks behind India’s, an indication of faster spread in Nepal than in India. It seems time was the only thing that separated Nepal and India epidemiologically for COVID-19. Time is catching up fast with Nepal.
The densely populated Terai region and valleys of Nepal, with proximity to India and greater movement of people, will initially likely experience a more severe impact from COVID-19 outbreak– i.e. disease and death– before the rural areas in the hilly and mountainous region are impacted. However, the recent media reports of several regional hospitals in densely populated Terai districts already reaching their capacity suggest that this trend has started. Based on my conversation with a person knowledgeable of public health data indicate that many districts in the hilly regions have also started experiencing increased COVID-19 cases and deaths.
Collapse of a Feeble Health System
Even during the best of times, the healthcare system in Nepal is not capable of dealing with many severe cases of illnesses. Most “hospitals” in Nepal are neither adequately equipped nor staffed to deal with severe COVID-19 cases. Efforts to add a few beds and ‘ventilators’ in provincial hospitals are essentially a good social media photo opportunity rather than having any meaningful impact on saving lives.
An increase in COVID-19 cases will collapse an already feeble health system in a matter of days and that appears to have started. In fact, on April 30, 2021, the Ministry of Health essentially declared the collapse of the health system when it issued a statement: “As the number of infections has been increasing, the health system is not able to cope and a situation has already arisen in which hospital beds cannot be made available” (The Kathmandu Post ). I am not surprised that the government finally admitted the obvious; I am surprised that they had not been beating that drum since the start of the pandemic. Unfortunately, Nepal likely is going to see a repeat of the scenes of disease and deaths currently playing out in India in the next few weeks. The COVID-19 crisis in Nepal is just beginning.
Even the most advanced health systems in the world are unlikely to handle an unrelenting tide of sickness. You simply cannot treat your way out of a pandemic. Public health measures to control infections must be in place to stem the tide of the incoming COVID-19 tsunami in Nepal. However, the existing public health infrastructure does not seem to have capable leadership, a functioning disease surveillance system, and effective prevention and control capabilities to tackle an incoming COVID-19 tsunami.
Why Did the Second Wave Happen?
The second wave in Nepal was neither unexpected nor surprising to epidemiologists. This situation is likely a result of a combination of factors including viral characteristics–potentially more infectious strains of the virus (e.g. the UK variant; the “double mutation” Indian variant) that likely enter Nepal through India– and environmental conditions– low humidity level that facilitates viral transmission and heavy air pollution in the region that can compromise the respiratory tract, and human behavior. While viral characteristics and environmental factors likely contributed, complacency likely is the primary driving force behind the second wave of COVID-19 in Nepal.
Because the first wave that peaked in October 2020 did not seem “that bad”, there may have been a sense that the worst of the pandemic was over. Complacency about the virus and its ongoing impact in Nepal likely set in among the political leaders and the general population. A February 11, 2021 story published in The Guardian aptly describe the national complacency following decline in COVID-19 cases after the first wave :
Traffic jams and soaring pollution levels are back. Political leaders are organizing mass rallies, far more focused on fighting each other than any virus. If poorer Nepalis are struggling with the dire economic fallout from Covid-19, on the surface, at least, it appears daily life in the capital, Kathmandu, is back to normal. “It’s as if nothing has happened. The nightclubs are crowded. Schools and colleges are reopening. Sports venues are full. It doesn’t seem like there is any Covid,” says Sameer Mani Dixit, a public health specialist. “It defies logic.”
It is wishful thinking, false bravado, or misguided optimism for any country to believe that they are not going to be affected by the COVID-19 pandemic and act like life was normal. A few months back, many in the media, as well as some public health experts, were trying to understand why India (and other developing countries) had not been as severely impacted by COVID-19 as the United States and many European countries. Many theories were being proposed, and reasons being speculated, about India’s apparent lower COVID-19 infection and mortality rates than many western countries.
Time as a factor was mostly ignored as one of the possible explanations. The disease transmission dynamic is going to be somewhat different depending on the demographic, environmental, and behavioral factors in each population. The virus is not going to follow an identical pattern of transmission in every population, and it is only a matter of time before the virus will spread widely in every population and cause substantial disease and death. Maybe new virus variants are contributing to the rise in cases in Nepal, but a general complacency about the risk of the pandemic to the Nepali population, thus ignoring basic public health guidelines and behaving as if everything was normal, explains a whole lot more. Complacency has tragic consequences.
Migrant workers returning home from India in the past two weeks (see The New York Times story) are again being blamed for the rise of cases in Nepal by many including some public health experts. In the last few months, there was a regular movement of people between the two countries. This movement included daily cross-border interactions, Indian tourists and pilgrims visiting Nepal, and Nepali pilgrims attending the Kumbha Mela festival in India (former King and Queen were infected during their visit) and can account for how the virus spread between the two places. In addition, the reckless behavior on the part of politicians and the general population in the last few months can likely account for the second wave of COVID-19 in Nepal without scapegoating migrant workers. Although many of the returning migrant workers are likely infected are contributing to total case load, the virus was already spreading in Nepal before migrant workers started returning from India in the past two weeks.
The Way Out through Public Health Measures
In the long run, vaccination is the way to come out of this pandemic. However, Nepal has a long way to go before a significant proportion of its 30 million people are vaccinated. The country has only vaccinated about 1.7 million people with the first dose and about 380,000 people with both doses of the AstraZeneca vaccine. The country was able to access and use 1 million doses donated by India and the rest purchased from the Serum Institute of India. However, with the raging epidemic in India and its decision to curtail vaccine export, the vaccine supply in Nepal has dwindled. A recent donation by China of about 800,000 doses of one of its vaccines, is good alternative but it is far short of the necessary doses to vaccinate enough people to have a significant impact on the current disease spread.
It will be a while (months, if we want to be really optimistic) before the vaccines are widely available in Nepal and other developing countries. In the short-term, for Nepal to rely on vaccines to save its people from COVID-19 reminds me of a Nepali proverb:
लास्सामा सुन छ, कान मेरा बुच्चै!
It basically expresses the sentiment that COVID-19 current vaccine availability in other countries are of little consequence for Nepal.
While there are multiple highly effective and safe vaccines for COVID-19, the reality is that supply is limited globally. Nepal, along with a large segment of the world, is going to have to wait until global vaccine production ramps up. Perhaps the euphoria surrounding the phenomenal results of COVID-19 vaccines in December 2020 and their emergency use authorization in the United States and other countries contributed to global COVID-19 complacency. Perhaps people globally, and in Nepal, had a mistaken belief that vaccines would be widely available and impact the pandemic immediately, thus creating a false sense of security and adding to the complacency.
In the short-term, Nepalis need to be realistic and seriously adopt the non-pharmaceutical public health measures—masking, social distancing, limiting gatherings and hand hygiene— to control the virus transmission and reduce disease and deaths. Until adequate supply of vaccines become available and administered to a significant proportion of the population, the only measures available to curtail the pandemic are these public health measures. They are very effective in reducing the risk of virus transmission, and consequently the severe disease and deaths. Correctly adopted by a large proportion of people in a community, these measures can be as effective as the COVID-19 vaccines.
The responsibility to make these public health measures work lies not only with the government, but with every citizen. Whether the government imposes a ‘lockdown’ or not, it is up to each individual citizen to do their part to slow the spread of the virus. People cannot behave as if life is normal—continue with weddings and festivals, parties and political rallies—and expect the virus to not spread. The odds of someone being infected increases with the increasing crowd size. The odds of virus transmission increase with decreasing size of an indoor space and related ventilation. If you don’t have to, you shouldn’t be gathering with anyone who does not live in the same household. People need to take a commonsense approach to these mitigation measures that have shown to work well.
Public health measures work only when public are seriously engaged in implementing those measures. A competent political leadership, that relies on science and logic matters because it can pull the public together in the same direction towards a common goal of mitigating the problem. It is the responsibility of the government and the leaders to provide sound public health guidelines and policies for the public. However, that is not enough, if the public is not engaged or, at worst, is behaving contrary to the accepted public health guidelines.
During a devastating pandemic, behaving as if things were normal does not make it so. It is incumbent upon people to realize that the coronavirus is an airborne pathogen that spreads when people engage in activities that bring infected and uninfected people together, especially in smaller and unventilated indoor spaces, without facial coverings, and for an extended time period. The virus relies on people to help it spread.
How people behave matters. Their actions will determine how bad this second wave ends up being and whether Nepal will have subsequent waves. The country will eventually have access to COVID-19 vaccines which will help to end the pandemic with reduced severe disease and deaths. Until then, the effective public health measures can protect people and avoid the need to find a hospital bed because of COVID-19. These hospital beds may or may not help to survive the disease anyway. Preventing an infection is much more under the control of an individual than surviving severe COVID-19.

Madhav P. Bhatta is a Professor of Epidemiology and Global Health at Kent State University College of Public Health. He received his Bachelor’s degree from the University of Pennsylvania and Masters of Public Health (Epidemiology and International Health) and PhD (Epidemiology) from the University of Alabama at Birmingham. He was born and raised in Nepal.
https://www.facebook.com/madhav.bhatta.90
https://www.linkedin.com/in/madhav-bhatta-093b3314/